For decades, a failing tooth with significant bone loss, gingival recession, or periapical infection carried a familiar prognosis: extraction, months of socket healing, bone augmentation, another healing period, maybe another soft tissue surgery and only then — implant placement. The standard timeline stretched to a year or more, involving multiple surgeries, considerable patient discomfort and tremendous cost.
That model is being replaced. The Immediate Dentoalveolar Restoration (IDR) protocol, developed by Dr. José Carlos da Rosa, collapses that entire sequence into a single surgical appointment. Extraction, flapless bone reconstruction, implant placement, and a provisional crown — all done at once, even in sockets that conventional protocols would consider contraindicated for immediate loading.
“What sounds challenging is a clear, sound biological concept which makes implant dentistry much simpler, safer, and faster.”
— Dr. José Carlos da Rosa, IDR Protocol Developer
What Is the IDR Protocol?
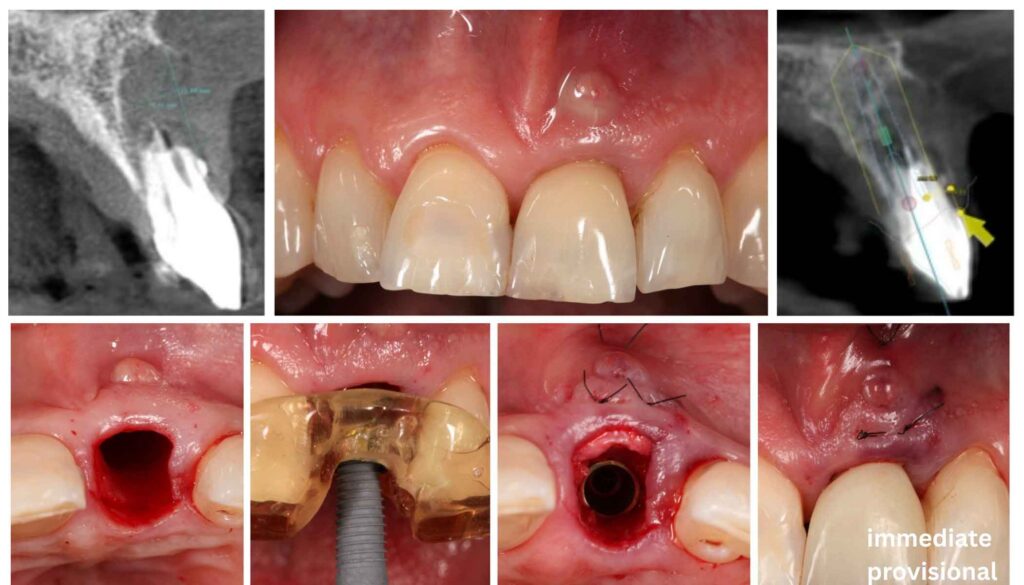
Immediate Dentoalveolar Restoration is a flapless, single-stage surgical approach that simultaneously addresses the hard and soft tissue deficiencies present in a compromised extraction socket while placing the implant and provisional crown.
The protocol is grounded in a fundamental insight from bone biology: the fresh extraction socket, with its intact vascular supply and inflammatory cascade already primed for regeneration, represents an ideal healing environment, if the right grafting material is introduced at the right moment.
The cornerstone of IDR is the use of autogenous cortico-cancellous bone harvested from the maxillary tuberosity. Unlike synthetic substitutes or freeze-dried allografts, tuberosity bone carries living osteoblasts and osteocytes with their vascular supply partially intact.
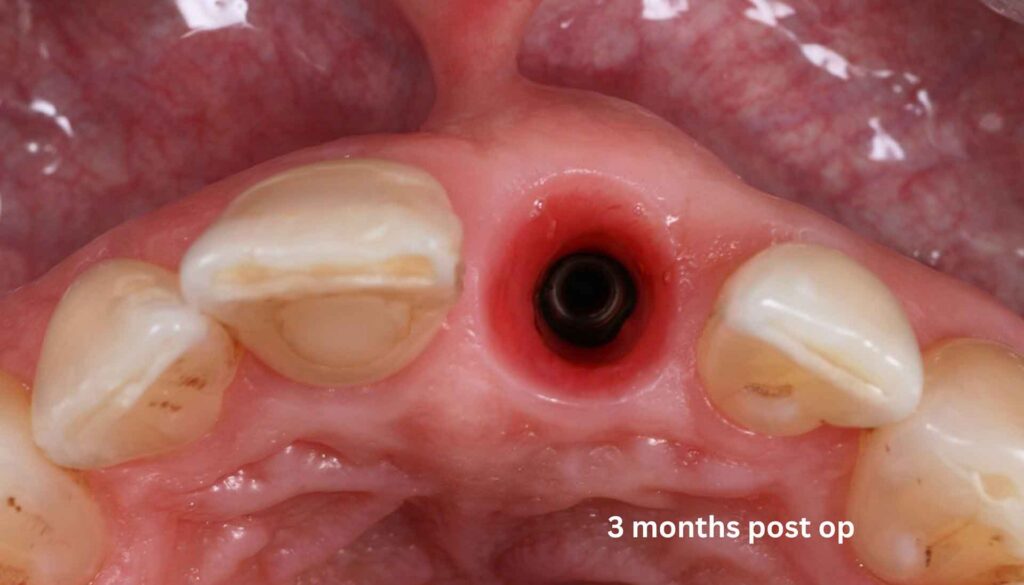
This “active bone” accelerates integration, demonstrates a natural immunological resistance to infection, and supports new bone formation at a pace that allows final implant loading in just three months, compared to the nine months or longer typical of conventional staged approaches.
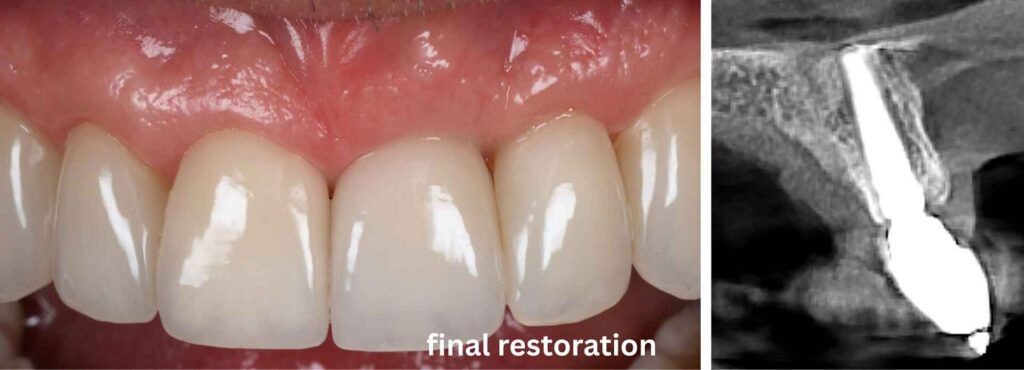
The Triple Graft: One Harvest Site, Three Tissue Types
One of the most elegant aspects of the IDR technique is the Triple Graft, in which cortico-cancellous bone, cancellous bone, and connective tissue are harvested simultaneously from a single tuberosity site. This eliminates the need for a second donor area, minimizes operative morbidity, and provides everything required for comprehensive three-dimensional tissue reconstruction in one pass.
The harvest procedure itself is minimally invasive and well tolerated by patients. Tuberosity typically has abundant cancellous bone with a high concentration of active marrow cells, making it the gold standard among autogenous intraoral donor sites for implant-related augmentation.
Socket Classification and Indications
A key strength of the IDR protocol is its breadth. Where conventional guidelines restrict immediate implants to “ideal” sockets with intact four-wall bone and no infection, IDR was specifically designed to address the full spectrum of clinical reality. Dr. da Rosa classifies compromised sockets and defines clear treatment pathways for each:
| Socket Type | Key Features | IDR Applicability |
| Intact socket | All four walls present, no recession, no infection | Standard IDR application |
| Buccal bone loss | Dehiscence or fenestration of the facial plate | Flapless reconstruction with cortico-cancellous graft |
| Gingival recession | Soft tissue deficiency at the facial aspect | Connective tissue component of Triple Graft |
| Active inflammation | Periapical pathology or chronic infection | IDR possible using tuberosity bone’s natural resistance |
| Loss of papilla | Interproximal soft tissue collapse | Addressed via emergence profile of provisional |
| 360° bone defect | Complete circumferential bone loss | Advanced IDR application — covered in course |
| Large incisor nerve canal | Nasopalatine canal proximity | Specific IDR variant taught in course |
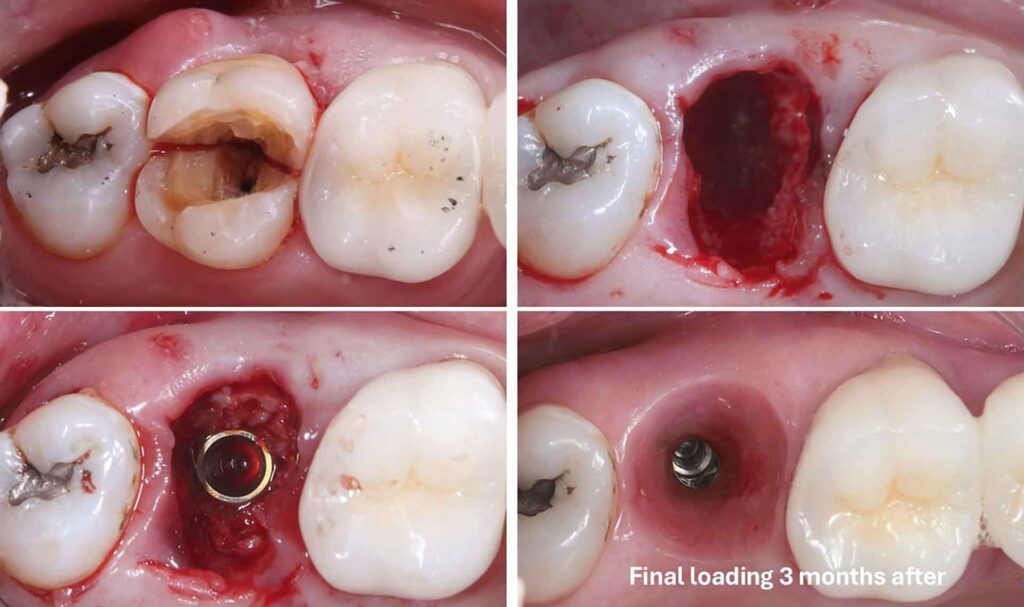
The Biological Foundation: Why Active Bone Changes Everything
Understanding why IDR works requires appreciating the hierarchy of bone grafting materials.
Hierarchy of bone grafting materials
At the top sits fresh autogenous bone with viable cells: osteogenic, osteoinductive, and osteoconductive all at once.
Below that lies processed allograft (osteoinductive/osteoconductive but acellular), then xenograft (osteoconductive only), and finally alloplastics (scaffold only).
The maxillary tuberosity occupies a uniquely favorable position in this hierarchy. It is a largely cancellous region with a rich marrow space populated by osteoprogenitor cells. When harvested and placed immediately into a fresh socket, these cells encounter an environment already flooded with growth factors, PDGF, BMP-2 and BMP-7, and an active blood supply, precisely the conditions they need to proliferate and differentiate rapidly into new bone.
Co-taught in the IDEA course, Dr. Luis Violin, a medical doctor and internationally recognized bone biology researcher, presents the latest scientific evidence underpinning these mechanisms, giving participants not just the “how” but the deep “why” that builds long-term clinical confidence.
KEY BIOLOGICAL ADVANTAGES OF TUBEROSITY BONE
- Contains living osteoblasts and osteoprogenitor cells (osteogenic)
- Rich in bone morphogenetic proteins BMP-2 and BMP-7 (osteoinductive)
- Provides a collagen scaffold for cell migration (osteoconductive)
- Natural immunological resistance to bacterial infection
- Enables final loading in ~3 months vs. 9+ months with staged approaches
- Minimal donor site morbidity – well tolerated by patients
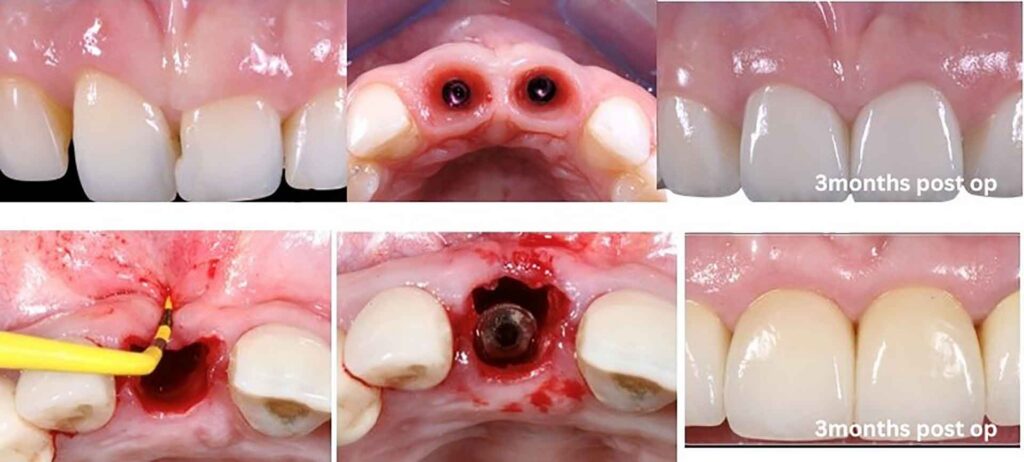
Surgical Protocol: Step by Step
While the nuances of patient selection, socket assessment, and digital planning are covered in depth during the IDEA course, the IDR protocol follows a logical sequence that becomes reproducible with hands-on training:
1. Pre-Surgical Assessment and Digital Planning
CBCT evaluation guides implant diameter selection — a paradigm shift from conventional thinking, as IDR uses the fresh socket anatomy differently than traditional protocols. Digital workflow integration allows virtual implant positioning, smile design preview, and fabrication of a provisional prosthesis before the surgery begins.
2. Atraumatic Extraction with Tissue Preservation
Periotomes, thin-bladed luxators, and rotational forces minimize trauma to the alveolar housing. The periosteum is left intact. No flap is raised. This flapless approach preserves the blood supply to the crestal bone — a critical factor in maintaining the buccal plate that is so often sacrificed in conventional extractions.
3. Socket Debridement and Implant Placement
After thorough curettage of granulation tissue and any infected material, the implant is placed with precise three-dimensional positioning. Tapered, deep-threaded implants with moderately to highly roughened surfaces are preferred to maximize primary stability in the incompletely healed socket environment.
4. Maxillary Tuberosity Harvest
Under local anesthesia, a minimally invasive approach exposes the tuberosity. Cortico-cancellous block, particulate cancellous bone, and connective tissue are harvested as the Triple Graft. The harvest site heals uneventfully and patients typically report minimal discomfort beyond the implant site itself.
5. Flapless Bone Reconstruction
The autogenous graft is packed into the gap between implant and socket walls, filling bony deficiencies and establishing a biological seal. Unlike membrane-covered grafting approaches that require a second surgery for membrane removal, the flapless IDR approach leaves the periosteum undisturbed, maintaining vascular continuity and greatly simplifying the post-operative course.
6. Emergence Profile Design and Provisional Restoration
A screw-retained provisional crown is placed at the time of surgery, restoring esthetics immediately and shaping the soft tissue emergence profile from day one. The provisional must be out of occlusal contact during the healing phase, but its presence guides the peri-implant gingival architecture toward the desired final form.
Outcomes: What the Evidence Shows

The IDR protocol is backed by peer-reviewed evidence spanning decades of Dr. da Rosa’s clinical research. Key outcome data demonstrate implant survival rates comparable to conventional staged protocols, superior preservation of buccal bone volume, and significantly shorter total treatment time.
The 3-month loading milestone, compared to the 9–18 months often required in staged augmentation cases, has profound implications for patient satisfaction and practice efficiency.
It is proven that immediate-autogenous, biology-driven implant placement does not experience any of the complications that conventional, multi-staged surgeries are experiencing. Therefore, it is not useful to compare both treatment approaches with each other.
The IDR technique is a low-risk and safe treatment concept which is truly simplifying implant dentistry to a high degree for dentists and their patients.
“It’s been incredible. Jose Carlos is showing us things that are definitely outside the box, with truly impressive results. I’ve been practicing for many years but over the past few days these techniques have really pushed me to think differently. This will absolutely influence my practice moving forward.”
— Joseph Kan, Periodontist, Loma Linda, CA
“I’m an Oral Surgeon, and I have done a lot of bone grafts but in an invasive way. Now, I have another approach with less invasive technique, saving time and being more effective.”
— Quang Phi Tran, Oral Surgeon, Ho Chi Minh City, Vietnam
“Thank you Dr. da Rosa for opening our minds to the possibilities and teaching us how to do it in ways that young practitioners, like me can apply in our daily practice. His methods are simplified into repeatable steps that can be perfected the more you do it.”
— Teresa Le, General Practitioner, Cudahy, CA
Who Should Learn the IDR Technique?

The IDR protocol is designed to be applicable across all levels of implant experience. General practitioners and prosthodontists expanding into implant surgery will find a systematic, reproducible protocol with a clear learning curve.
Specialists, periodontists and oral surgeons will discover new powerful treatment options for cases they currently stage over many months.
The course is explicitly structured to meet each clinician where they are, with a 1:8 instructor-to-participant ratio ensuring individualized training throughout every hands-on session.
Very valuable is the after-course mentorship by Dr. da Rosa to guide each participant individually on their patients through treatment planning and surgical steps.
About Dr. José Carlos da Rosa

Dr. da Rosa is the creator of the IDR technique and lead author of the internationally recognized Quintessence Publishing bestseller Immediate Dentoalveolar Restoration: Immediately Loaded Implants in Compromised Sockets, now in its second edition.
With decades of clinical experience and a body of peer-reviewed research, he brings both the theoretical depth and practical precision that define IDEA’s world-class faculty.
What You Will Master after the IDEA Course in Your Clinic
“There were 3 WOW factors in this course:
The 1st WOW is when Dr. da Rosa showed a case which seemed almost impossible to do immediate implant placement and there it is – case achieved.
The 2nd WOW is the long-term follow-up of such outstanding cases, 10 – 20-year follow-ups with amazing results.
And the 3rd WOW factor, these cases are broken down in such simplicity that I can go back next week and apply to my patients.
Thank you for your generosity and kindness in sharing all these cases.”
— Samuel Koo, Periodontist, Wellesley Hills, MA
COURSE LEARNING OBJECTIVES
- Diagnose and classify compromised sockets and alveolar bone defects
- Apply the full IDR protocol step by step, from simple to complex cases
- Select optimal implant diameter for post-extraction placement
- Understand bone biology from a higher perspective – by Dr. Luis Violin
- Harvest autogenous Triple Grafts from the maxillary tuberosity
- Perform flapless, minimally invasive surgery for immediate implant placement
- Design and place ideal provisional restorations with correct emergence profiles
- Integrate digital CBCT planning and guided workflow into IDR cases
- Manage complications — taught by Dr. Luis Violin
Course Details — Register Today

Instructor: José Carlos da Rosa, D.D.S., M.Sc., Ph.D.
IDEA Academy’s 4-day intensive hands-on CE course is capped at just 16 participants with a 1:8 instructor-to-student ratio, allowing the instructors to easily adapt to your educational needs.
The all-inclusive package covers 5-night, hotel accommodation, local transportation, and in-house chef meals. The only additional cost is your flight.
Dates: June 17–20, 2026 | 36 CE Credits | San Francisco Bay Area, California
Group Size: Maximum 16 participants

